2/12—CDC Task Force: Building Confidence in COVID-19 Vaccines
CDC Vaccine Task Force: Building Confidence in COVID-19 Vaccines Among Your Patients
COVID-19 vaccines; mRNA vaccine technology; safety monitoring; elements of vaccine confidence; strategies for building vaccine confidence; strategies for talking with patients about COVID-19 vaccine.
Strategies for addressing vaccine hesitancy - A systematic review [2015]
Across the literature, few strategies to address vaccine hesitancy were found to have been evaluated for impact on either vaccination uptake and/or changes in knowledge, awareness or attitude (only 14% of peer reviewed and 25% of grey literature). Thirteen relevant studies were used for the GRADE assessment that indicated evidence of moderate quality for the use of social mobilization, mass media, communication tool-based training for health-care workers, non-financial incentives and reminder/recall-based interventions. Overall, our results showed that multicomponent and dialogue-based interventions were most effective. However, given the complexity of vaccine hesitancy and the limited evidence available on how it can be addressed, identified strategies should be carefully tailored according to the target population, their reasons for hesitancy, and the specific context.
A Rapid Systematic Review of Public Responses to Health Messages Encouraging Vaccination against Infectious Diseases in a Pandemic or Epidemic
A rapid systematic review was performed. Thirty-five articles were included. Evidence from moderate to high quality studies for improving vaccine uptake included providing information about virus risks and vaccination safety, as well as addressing vaccine misunderstandings, offering vaccination reminders, including vaccination clinic details, and delivering mixed media campaigns across hospitals or communities. Behavioural influences (beliefs and intentions) were improved when: shorter, risk-reducing or relative risk framing messages were used; the benefits of vaccination to society were emphasised; and beliefs about capability and concerns among target populations (e.g., vaccine safety) were addressed. Clear, credible, messages in a language target groups can understand were associated with higher acceptability.
Influenza Vaccination Quality Improvement as a Model for COVID-19 Prophylaxis
This study was performed at an outpatient allergy and clinical immunology practice (MSBI) with hospital affiliation in New York City, New York. 984 patients met inclusion criteria, with a normal distribution of ages (18-80), race, and sex. Average vaccination rates prior to the intervention were 9.25-13.60%. The average vaccination rate after the intervention was 91.34%.
The public’s role in COVID-19 vaccination: Human-centered recommendations to enhance pandemic vaccine awareness, access, and acceptance in the United States
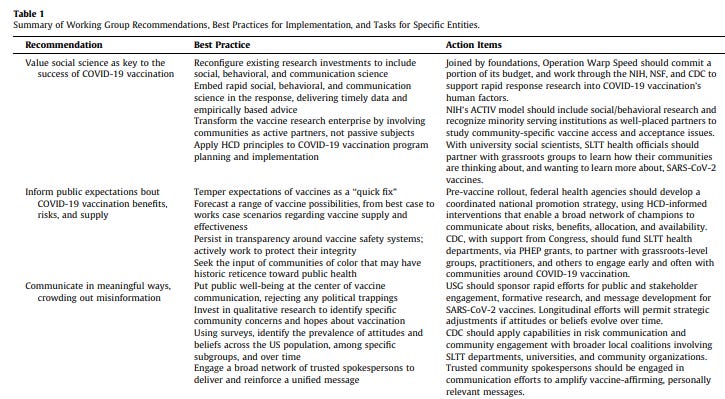
The research and recommendations presented in this paper are a product of the 23-person Working Group on Readying Populations for COVID-19 Vaccine (Table 1 ). This group was convened in April 2020 by principal investigators from the Johns Hopkins Center for Health Security and the Texas State University Department of Anthropology. [See also full report by the Johns Hopkins and 2-page summary.]
Missed an update? View past issues.