4/14—Outdoor Transmission: A Systematic Review
Outdoor Transmission of SARS-CoV-2 and Other Respiratory Viruses: A Systematic Review
We conducted a systematic review of peer-reviewed papers indexed in PubMed, EMBASE, and Web of Science and preprints in Europe PMC through 12 August 2020. Five identified studies found a low proportion of reported global SARS-CoV-2 infections occurred outdoors (<10%) and the odds of indoor transmission was very high compared to outdoors (18.7 times; 95% confidence interval, 6.0–57.9). In general, factors such as duration and frequency of personal contact, lack of personal protective equipment, and occasional indoor gathering during a largely outdoor experience were associated with outdoor reports of infection.
Single-dose administration and the influence of the timing of the booster dose on immunogenicity and efficacy of ChAdOx1 nCoV-19 (AZD1222) vaccine: a pooled analysis of four randomised trials
Between April 23 and Dec 6, 2020, 24 422 participants were recruited and vaccinated across the four studies, of whom 17 178 were included in the primary analysis (8597 receiving ChAdOx1 nCoV-19 and 8581 receiving control vaccine). Overall vaccine efficacy more than 14 days after the second dose was 66·7% (95% CI 57·4–74·0). There were no hospital admissions for COVID-19 in the ChAdOx1 nCoV-19 group after the initial 21-day exclusion period, and 15 in the control group. There were seven deaths considered unrelated to vaccination (two in the ChAdOx1 nCov-19 group and five in the control group), including one COVID-19-related death in one participant in the control group. In the participants who received two standard doses, after the second dose, efficacy was higher in those with a longer prime-boost interval (vaccine efficacy 81·3% [95% CI 60·3–91·2] at ≥12 weeks) than in those with a short interval (vaccine efficacy 55·1% [33·0–69·9] at <6 weeks). These observations are supported by immunogenicity data that showed binding antibody responses more than two-fold higher after an interval of 12 or more weeks compared with an interval of less than 6 weeks in those who were aged 18–55 years (GMR 2·32 [2·01–2·68]). A 3-month dose interval might have advantages over a programme with a short dose interval for roll-out of a pandemic vaccine to protect the largest number of individuals in the population as early as possible when supplies are scarce, while also improving protection after receiving a second dose.
Single-dose Oxford–AstraZeneca COVID-19 vaccine followed by a 12-week booster
Merryn Voysey and colleagues report the updated primary efficacy results for the Oxford–AstraZeneca ChAdOx1 nCoV-19 (AZD1222) vaccine from three single-blind, randomised controlled trials in the UK and Brazil and one double-blind study in South Africa. The study is based on an updated analysis of 17 178 participants (9696 [56·4%] were women, 12 975 [75·5%] were white, and 14 413 [83·9%] were aged 18–55 years, 1792 [10·4%] aged 56–69 years, and 973 [5·7%] aged 70 years or older) from the four trials. Overall, the value of this study is in providing evidence that a single dose of the ChAdOx1 nCoV-19 vaccine is highly efficacious in the 90 days after vaccination, that a longer prime-boost interval results in higher vaccine efficacy, and that protection against symptomatic COVID-19 is maintained despite a longer dosing interval. It offers much-needed evidence for the UK policy of extending the dosing interval to 12 weeks and for rapid mass-immunisation campaigns worldwide.
Genomic characteristics and clinical effect of the emergent SARS-CoV-2 B.1.1.7 lineage in London, UK: a whole-genome sequencing and hospital-based cohort study
Of 496 patients with samples positive for SARS-CoV-2 on PCR and who met inclusion criteria, 341 had samples that could be sequenced. 198 (58%) of 341 had B.1.1.7 infection and 143 (42%) had non-B.1.1.7 infection. We found no evidence of an association between severe disease and death and lineage (B.1.1.7 vs non-B.1.1.7) in unadjusted analyses (prevalence ratio [PR] 0·97 [95% CI 0·72–1·31]), or in analyses adjusted for hospital, sex, age, comorbidities, and ethnicity (adjusted PR 1·02 [0·76–1·38]). We did not identify an association of the variant with severe disease in this hospitalised cohort.
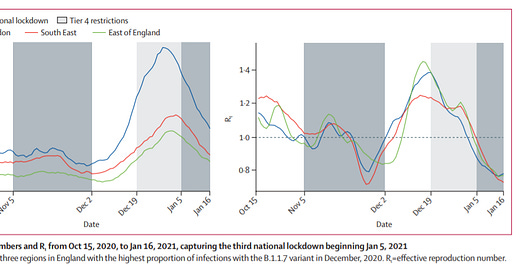
Changes in symptomatology, reinfection, and transmissibility associated with the SARS-CoV-2 variant B.1.1.7: an ecological study
From Sept 28 to Dec 27, 2020, positive COVID-19 tests were reported by 36 920 COVID Symptom Study app users whose region was known and who reported as healthy on app sign-up. We found no changes in reported symptoms or disease duration associated with B.1.1.7. For the same period, possible reinfections were identified in 249 (0·7% [95% CI 0·6–0·8]) of 36 509 app users who reported a positive swab test before Oct 1, 2020, but there was no evidence that the frequency of reinfections was higher for the B.1.1.7 variant than for pre-existing variants. We found a multiplicative increase in the Rt of B.1.1.7 by a factor of 1·35 (95% CI 1·02–1·69) relative to pre-existing variants. However, Rt fell below 1 during regional and national lockdowns, even in regions with high proportions of infections with the B.1.1.7 variant. The lack of change in symptoms identified in this study indicates that existing testing and surveillance infrastructure do not need to change specifically for the B.1.1.7 variant. In addition, given that there was no apparent increase in the reinfection rate, vaccines are likely to remain effective against the B.1.1.7 variant.