4/9—B.1.1.7: Reduced neutralization, but "widespread escape" from antibodies not observed
Reduced neutralization of SARS-CoV-2 B.1.1.7 variant by convalescent and vaccine sera
Variant B.1.1.7, now dominant in the UK, with increased transmission, harbors 9 amino acid changes in the spike, including N501Y in the ACE2 interacting surface. We examine the ability of B.1.1.7 to evade antibody responses elicited by natural SARS-CoV-2 infection or vaccination. We map the impact of N501Y by structure/function analysis of a large panel of well-characterized monoclonal antibodies. B.1.1.7 is harder to neutralize than parental virus, compromising neutralization by some members of a major class of public antibodies through light-chain contacts with residue 501. However, widespread escape from monoclonal antibodies or antibody responses generated by natural infection or vaccination was not observed.
Interim Estimates of Vaccine Effectiveness of BNT162b2 and mRNA-1273 COVID-19 Vaccines in Preventing SARS-CoV-2 Infection Among Health Care Personnel, First Responders, and Other Essential and Frontline Workers — Eight U.S. Locations, December 2020–March 2021
Prospective cohorts of 3,950 health care personnel, first responders, and other essential and frontline workers completed weekly SARS-CoV-2 testing for 13 consecutive weeks. Under real-world conditions, mRNA vaccine effectiveness of full immunization (≥14 days after second dose) was 90% against SARS-CoV-2 infections regardless of symptom status; vaccine effectiveness of partial immunization (≥14 days after first dose but before second dose) was 80%.
Association between living with children and outcomes from covid-19: OpenSAFELY cohort study of 12 million adults in England
Among 9 334 392 adults aged 65 years and under, during wave 1, living with children was not associated with materially increased risks of recorded SARS-CoV-2 infection, covid-19 related hospital or intensive care admission, or death from covid-19. In wave 2, among adults aged 65 years and under, living with children of any age was associated with an increased risk of recorded SARS-CoV-2 infection (hazard ratio 1.06 (95% confidence interval 1.05 to 1.08) for living with children aged 0-11 years; 1.22 (1.20 to 1.24) for living with children aged 12-18 years) and covid-19 related hospital admission (1.18 (1.06 to 1.31) for living with children aged 0-11; 1.26 (1.12 to 1.40) for living with children aged 12-18). Living with children aged 0-11 was associated with reduced risk of death from both covid-19 and non-covid-19 causes in both waves; living with children of any age was also associated with lower risk of dying from non-covid-19 causes. In contrast to wave 1, evidence existed of increased risk of reported SARS-CoV-2 infection and covid-19 outcomes among adults living with children during wave 2. However, this did not translate into a materially increased risk of covid-19 mortality, and absolute increases in risk were small.
Sharing a household with children and risk of COVID-19: a study of over 300 000 adults living in healthcare worker households in Scotland
241 266, 41 198, 23 783 and 3850 adults shared a household with 0, 1, 2 and 3 or more young children, respectively. Over the study period, the risk of COVID-19 requiring hospitalisation was reduced progressively with increasing numbers of household children—fully adjusted HR (aHR) 0.93 per child (95% CI 0.79 to 1.10). The risk of any COVID-19 was similarly reduced, with the association being statistically significant (aHR per child 0.93; 95% CI 0.88 to 0.98). After schools reopened to all children in August 2020, no association was seen between exposure to young children and risk of any COVID-19 (aHR per child 1.03; 95% CI 0.92 to 1.14). Between March and October 2020, living with young children was associated with an attenuated risk of any COVID-19 and COVID-19 requiring hospitalisation among adults living in healthcare worker households.
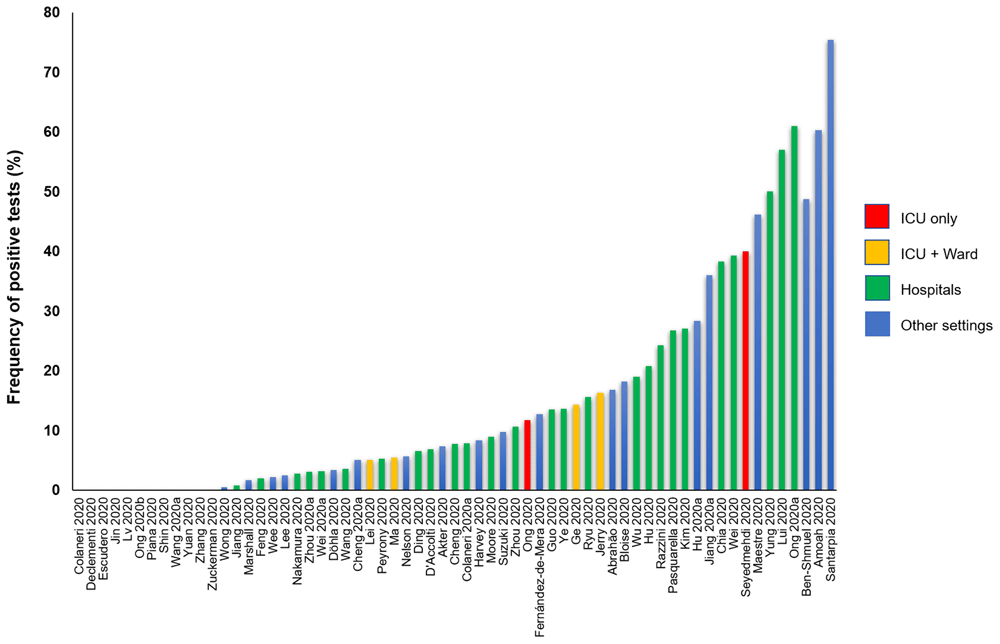
SARS-CoV-2 and the role of fomite transmission: a systematic review
[Preprint.] We found 64 studies: 63 primary studies and one systematic review (n=35). The settings for primary studies were predominantly in hospitals (69.8%) including general wards, ICU and SARS-CoV-2 isolation wards. The frequency of positive SARS-CoV-2 tests across 51 studies (using RT-PCR) ranged from 0.5% to 75%. Cycle threshold values ranged from 20.8 to 44.1. Eleven studies (17.5%) attempted viral culture, but none found a cytopathic effect. The majority of studies report identification of SARS-CoV-2 RNA on inanimate surfaces; however, there is a lack of evidence demonstrating the recovery of viable virus.