Critical exposure time in a small indoor space is less than 1 h
Estimate of the critical exposure time based on 70 confirmed COVID-19 cases
This study evaluates the critical ventilation rates according to room size and exposure time when a susceptible person is in the same room as an infector. The analytical results were based on data obtained from 70 confirmed COVID-19 cases transmitted in confined spaces without an operational ventilation system. The results reveal that even with active ventilation (20 h−1 air exchange rate), the critical exposure time for a susceptible person with a COVID-19 infector in a small space of 20 m3 is less than 1 h.
Accepting Restrictions and Compliance With Recommended Preventive Behaviors for COVID-19: A Discussion Based on the Key Approaches and Current Research on Fear Appeals
Whilst the majority follow the rules and recommendations with great care, others are more lax or simply refuse to comply. These differences might be accounted for according to a number of factors including personal, social, cultural, mental, and economic variables. Being persuaded to comply with preventive rules, especially those concerned with health-related behaviors, also bring certain other factors into play. Fear is one of those factors, and is one of the most powerful. It is well known that fear-based appeals can be effective in inculcating health behaviors, with many theories having been developed in this area. However, both the content of the message (the level of the fear it contains) and certain personal variables can determine the persuasive power of the fear appeal. It can even have an adverse effect if not properly applied.
SARS-CoV-2 seroprevalence among blood donors in Québec, and analysis of symptoms associated with seropositivity: a nested case-control study
A total of 7691 blood donors were included in the study. After adjustments, the seroprevalence rate was 2.2% (95% CI 1.9–2.6). Seropositive donors reported one or more symptoms in a proportion of 52.2% (95% CI 44.2–60.1); this proportion was 19.1% (95% CI 13.4–26.1) among seronegative donors, suggesting that approximately 50–66% of all infections were asymptomatic. Assuming that blood donors are fairly representative of the general adult population, this study shows that less than 3% of 18–69-year-olds have been infected during the first wave of the pandemic in the province of Québec.
Individuals who were mildly symptomatic following infection with SARS-CoV-2 B.1.1.28 have neutralizing antibodies to the P.1 variant
[Preprint.] Convalescent sera from 60 individuals following a documented SARS-CoV-2 infection were assayed for neutralizing antibody titer against both strains. Fifty-six and 50 sera were positive for neutralizing antibodies against the ancestral and P.1 strains, respectively. Neutralization titers were higher against the ancestral strain, but in the majority of patients differences did not differ by more than a single dilution. Neutralizing antibodies that were generated following infection with SARS-CoV-2 B.1.1.28 were effective in vitro, against the SARS-CoV-2 P.1. variant.
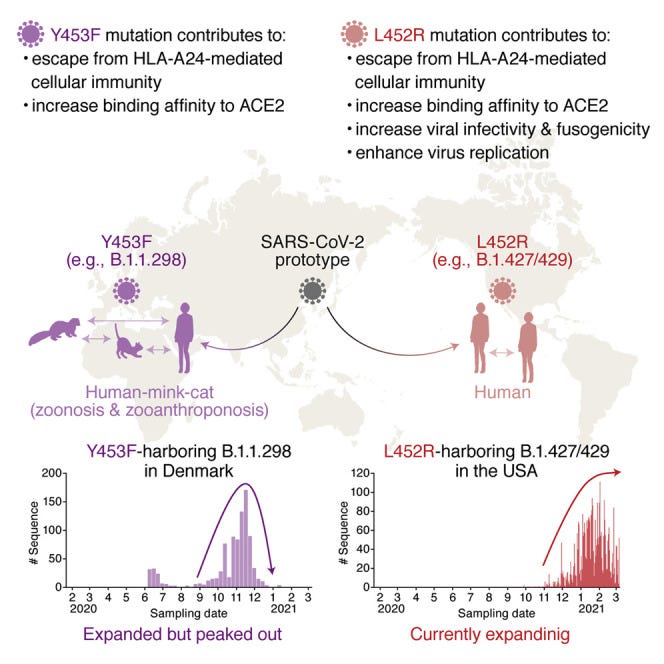
SARS-CoV-2 spike L452R variant evades cellular immunity and increases infectivity
Here, we demonstrate that two recently emerging mutations in the receptor-binding domain of the SARS-CoV-2 spike protein, L452R (in B.1.427/429 and B.1.617) and Y453F (in B.1.1.298), confer escape from HLA-A24-restricted cellular immunity. These mutations reinforce affinity toward the host entry receptor ACE2. Notably, the L452R mutation increases spike stability, viral infectivity, viral fusogenicity, and thereby promotes viral replication. These data suggest that HLA-restricted cellular immunity potentially affects the evolution of viral phenotypes and that a further threat of the SARS-CoV-2 pandemic is escape from cellular immunity.