Efficient border testing via reinforcement learning
Efficient and targeted COVID-19 border testing via reinforcement learning
We report the design and performance of a reinforcement learning system, nicknamed ‘Eva’. In the summer of 2020, Eva was deployed across all Greek borders to limit the influx of asymptomatic travellers infected with SARS-CoV-2. In contrast to country-wide protocols, Eva allocated Greece’s limited testing resources based upon incoming travellers’ demographic information and testing results from previous travellers. By comparing Eva’s performance against modelled counterfactual scenarios, we show that Eva identified 1.85 times as many asymptomatic, infected travellers as random surveillance testing, with up to 2-4 times as many during peak travel, and 1.25-1.45 times as many asymptomatic, infected travellers as testing policies that only utilize epidemiological metrics. Our results raise serious concerns on the effectiveness of country-agnostic internationally proposed border control policies that are based on population-level epidemiological metrics.
Air travel-related outbreak of multiple SARS-CoV-2 variants
Background. A large cluster of 59 cases were linked to a single flight with 146 passengers from New Delhi to Hong Kong in April 2021. Methods. Epidemiological information. Whole genome sequencing. Results. Sequence analysis identified six lineages of SARS-CoV-2 belonging to two variants of concern (Alpha and Delta) and one variant of public health interest (Kappa) involved in this outbreak. Phylogenetic analysis confirmed at least three independent sub-lineages of Alpha with limited onward transmission, a superspreading event comprising 37 cases of Kappa, and transmission of Delta to only one passenger. Conclusions. Requiring a nucleic acid test within 72 hours of departure may be insufficient to prevent importation or in-flight transmission.
The impact of heating, ventilation and air conditioning (HVAC) design features on the transmission of viruses, including SARS-CoV-2: an overview of reviews
[Preprint.] Searching identified 361 citations, 45 were potentially relevant, and 7 were included. Reviews were published between 2007 and 2021, and included 47 virus studies. Two earlier reviews (2007, 2016) of 21 studies found sufficient evidence that mechanical ventilation (airflow patterns, ventilation rates) plays a role in airborne transmission; however, both found insufficient evidence to quantify minimum mechanical ventilation requirements. One review (2017) of 9 studies examining humidity and indoor air quality found that influenza virus survival was lowest between 40% and 80% relative humidity; authors noted that ventilation rates were a confounding variable. Two reviews (2021) examined mitigation strategies for coronavirus transmission, finding droplet transmission decreased with increasing temperature and relative humidity. One review (2020) identified 14 studies examining coronavirus transmission in air-conditioning systems, finding HVAC systems played a role in virus spread during previous coronavirus outbreaks. One review (2020) examined virus transmission interventions on public ground transportation, finding ventilation and filtration to be effective. Seven reviews synthesizing 47 studies demonstrate a role of HVAC in mitigating airborne virus transmission.
Effects of adding L-arginine orally to standard therapy in patients with COVID-19: A randomized, double-blind, placebo-controlled, parallel-group trial. Results of the first interim analysis
This is a parallel-group, double-blind, randomized, placebo-controlled trial conducted on patients hospitalized for severe COVID-19. Patients received 1.66 g L-arginine twice a day or placebo, administered orally. No treatment-emergent serious adverse events were attributable to L-arginine. At 10-day evaluation, 71.1% of patients in the L-arginine arm and 44.4% in the placebo arm (p < 0.01) had the respiratory support reduced; however, a significant difference was not detected 20 days after randomization. Strikingly, patients treated with L-arginine exhibited a significantly reduced in-hospital stay vs placebo, with a median (interquartile range 25th,75th percentile) of 46 days (45,46) in the placebo group vs 25 days (21,26) in the L-arginine group (p < 0.0001). In this interim analysis, adding oral L-arginine to standard therapy in patients with severe COVID-19 significantly decreases the length of hospitalization and reduces the respiratory support at 10 but not at 20 days after starting the treatment.
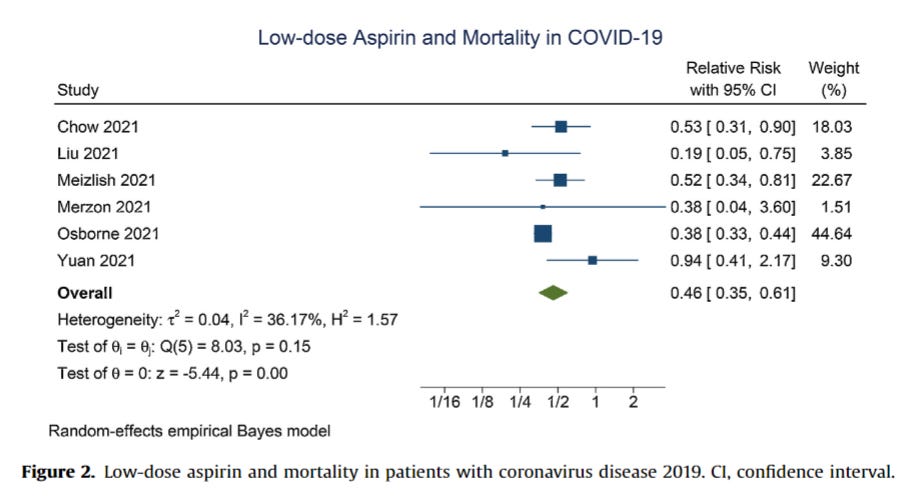
Active prescription of low-dose aspirin during or prior to hospitalization and mortality in COVID-19: A systematic review and meta-analysis of adjusted effect estimates
Six eligible studies were included in this meta-analysis, comprising 13,993 patients. The studies had low-to-moderate risk of bias based on the Newcastle–Ottawa Scale. The meta-analysis indicated that the use of low-dose aspirin was independently associated with reduced mortality {RR 0.46 [95% confidence interval (CI) 0.35–0.61], P < 0.001; I2 = 36.2%}. Subgroup analysis on in-hospital low-dose aspirin administration also showed a significant reduction in mortality [RR 0.39 (95% CI 0.16–0.96), P < 0.001; I2 = 47.0%]. Use of low-dose aspirin is independently associated with reduced mortality in patients with COVID-19, with low certainty of evidence.