EU adds another rare side effect to AstraZeneca shot
EU adds another rare blood condition as side effect of AstraZeneca shot
[Media report.] Europe's drug regulator on Friday identified another very rare blood condition as a potential side effect of AstraZeneca's (AZN.L) COVID-19 vaccine and said it was looking into cases of heart inflammation after inoculation with all coronavirus shots. The European Medicines Agency's (EMA) safety committee said that capillary leak syndrome (CLS) must be added as a new side effect to labelling on AstraZeneca's vaccine. People who had previously sustained the condition, where fluids leak from the smallest blood vessels causing swelling and a drop in blood pressure, should not receive the shot, the EMA added.
COVID-19 outbreaks following full reopening of primary and secondary schools in England: Cross-sectional national surveillance, November 2020
Primary and secondary schools reporting an outbreak (≥2 laboratory-confirmed cases within 14 days) to Public Health England (PHE) between 31 August and 18 October 2020 were contacted. There were 969 school outbreaks reported to PHE, comprising 2% (n = 450) of primary schools and 10% (n = 519) of secondary schools in England. Outbreaks were larger and across more year groups in secondary schools than in primary schools. Teaching staff were more likely to be the index case in primary (48/100, 48%) than secondary (25/79, 32%) school outbreaks (P = 0.027). When an outbreak occurred, attack rates were higher in staff (881/17,362; 5.07; 95%CI, 4.75–5.41) than students, especially primary school teaching staff (378/3852; 9.81%; 95%CI, 8.90–10.82%) compared to secondary school teaching staff (284/7146; 3.97%; 95%CI, 3.79–5.69%). Secondary school students (1105/91,919; 1.20%; 95%CI, 1.13–1.28%) had higher attack rates than primary school students (328/39,027; 0.84%; 95%CI, 0.75–0.94%). A higher proportion of secondary schools than primary schools reported a COVID-19 outbreak and experienced larger outbreaks across multiple school year groups. The higher attack rate among teaching staff during an outbreak, especially in primary schools, suggests that additional protective measures may be needed.
The impact of primary care supported shielding on the risk of mortality in people vulnerable to COVID-19: English sentinel network matched cohort study
A retrospective cohort study using a nationally representative English primary care database comparing people aged >= 40 years who were recorded as being advised to shield using a fixed ratio of 1:1, matching to people with the same diagnoses not advised to shield (n = 77,360 per group). We found a time-varying HR of mortality between groups. In the first 21 days, the mortality risk in people shielding was half those not (HR = 0.50, 95%CI:0.41–0.59. p < 0.0001). Over the remaining nine weeks, mortality risk was 54% higher in the shielded group (HR=1.54, 95%CI:1.41–1.70, p < 0.0001). Beyond the shielding period, mortality risk was over two-and-a-half times higher in the shielded group (HR=2.61, 95%CI:2.38–2.87, p < 0.0001). Shielding halved the risk of mortality for 21 days. Mortality risk became higher across the remainder of the shielding period, rising to two-and-a-half times greater post-shielding. Shielding may be beneficial in the next wave of COVID-19.
SARS-CoV-2 Superspread in Fitness Center, Hong Kong, China, March 2021
We used genomic sequencing to analyze 102 reverse transcription PCR–confirmed cases of SARS-CoV-2. Our finding highlights the risk for virus transmission in confined spaces with poor ventilation and limited public health interventions.
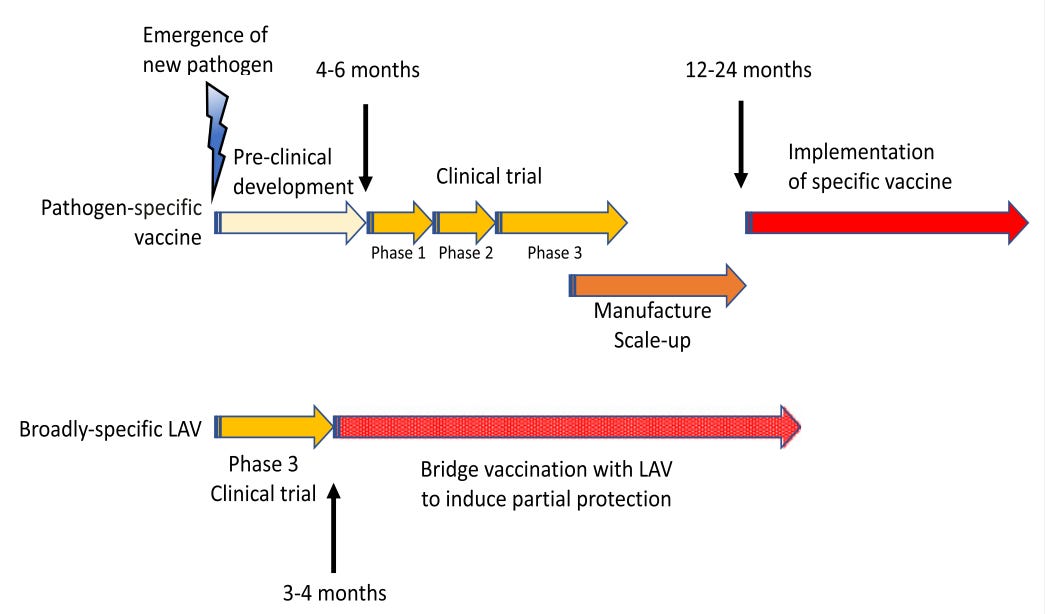
Old vaccines for new infections: Exploiting innate immunity to control COVID-19 and prevent future pandemics
Innate immunity is fundamental to mammalian host defense capacity to combat infections. Epidemiological and biological evidence suggests that the live-attenuated vaccines (LAV) targeting tuberculosis, measles, and polio induce protective innate immunity by a newly described form of immunological memory termed “trained immunity.” An LAV designed to induce adaptive immunity targeting a particular pathogen may also induce innate immunity that mitigates other infectious diseases, including COVID-19, as well as future pandemic threats. The broad protection induced by LAVs would not be compromised by potential antigenic drift (immune escape) that can render viruses resistant to specific vaccines.