New Dog Coronavirus Isolated from Pneumonia Patient in Malaysia
Novel Canine Coronavirus Isolated from a Hospitalized Pneumonia Patient, East Malaysia
We found canine CoV (CCoV) RNA in nasopharyngeal swabs from eight (2.5%) of 301 patients hospitalized with pneumonia during 2017-18 in Sarawak, Malaysia. Most patients were children living in rural areas with frequent exposure to domesticated animals and wildlife. Two of eight specimens contained sufficient amounts of CCoVs as confirmed by less-sensitive single-step RT-PCR assays, and one specimen demonstrated cytopathic effects (CPE) in A72 cells. Complete genome sequencing of the virus causing CPE identified it as a novel canine-feline recombinant alphacoronavirus (genotype II) that we named CCoV-HuPn-2018. Our findings underscore the public health threat of animal CoVs and a need to conduct better surveillance for them.
Heterologous prime-boost COVID-19 vaccination: initial reactogenicity data
In light of changing recommendations regarding use of the ChAdOx1 nCoV-19 (ChAd) COVID-19 vaccine (Vaxzevria, AstraZeneca), several countries are now advising that individuals previously primed with this vaccine should now receive an alternative vaccine as their second dose, most commonly mRNA vaccines. Both heterologous vaccine schedules induced greater systemic reactogenicity following the boost dose than their homologous counterparts, with feverishness reported by 37 (34%) of 110 recipients of ChAd for prime and BNT for boost compared with 11 (10%) of 112 recipients of ChAd for both prime and boost (difference 24%, 95% CI 13-35%). Feverishness was reported by 47 (41%) of 114 recipients of BNT for prime and ChAd for boost, compared with 24 (21%) of 112 recipients of BNT for both prime and boost (difference 21%, 95% CI 8-33%). Similar increases were observed for chills, fatigue, headache, joint pain, malaise, and muscle ache (figure; appendix). There were no hospitalisations due to solicited symptoms, and most of this increase in reactogenicity was observed in the 48 h after immunisation (appendix). Pending availability of a more complete safety dataset and immunogenicity results for heterologous prime-boost schedules (to be reported shortly), these data suggest that the two heterologous vaccine schedules in this trial might have some short-term disadvantages.
Effectiveness of the Pfizer-BioNTech and Oxford-AstraZeneca vaccines on covid-19 related symptoms, hospital admissions, and mortality in older adults in England: test negative case-control study
Participants: 156 930 adults aged 70 years and older who reported symptoms of covid-19 between 8 December 2020 and 19 February 2021. Results: Participants aged 80 years and older vaccinated with BNT162b2 before 4 January 2021 had a higher odds of testing positive for covid-19 in the first nine days after vaccination (odds ratio up to 1.48, 95% confidence interval 1.23 to 1.77), indicating that those initially targeted had a higher underlying risk of infection. Vaccine effectiveness was therefore compared with the baseline post-vaccination period. Vaccine effects were noted 10 to 13 days after vaccination, reaching a vaccine effectiveness of 70% (95% confidence interval 59% to 78%), then plateauing. From 14 days after the second dose a vaccination effectiveness of 89% (85% to 93%) was found compared with the increased baseline risk. Participants aged 70 years and older vaccinated from 4 January (when ChAdOx1-S delivery commenced) had a similar underlying risk of covid-19 to unvaccinated individuals. With BNT162b2, vaccine effectiveness reached 61% (51% to 69%) from 28 to 34 days after vaccination, then plateaued. With ChAdOx1-S, effects were seen from 14 to 20 days after vaccination, reaching an effectiveness of 60% (41% to 73%) from 28 to 34 days, increasing to 73% (27% to 90%) from day 35 onwards. On top of the protection against symptomatic disease, a further 43% (33% to 52%) reduced risk of emergency hospital admission and 51% (37% to 62%) reduced risk of death was observed in those who had received one dose of BNT162b2. Participants who had received one dose of ChAdOx1-S had a further 37% (3% to 59%) reduced risk of emergency hospital admission. Follow-up was insufficient to assess the effect of ChAdOx1-S on mortality. Combined with the effect against symptomatic disease, a single dose of either vaccine was about 80% effective at preventing admission to hospital with covid-19 and a single dose of BNT162b2 was 85% effective at preventing death with covid-19.
Reinfection by the SARS-CoV-2 P.1 variant in blood donors in Manaus, Brazil
[Preprint.] We tested serial samples from 238 unvaccinated repeat blood donors using a SARS-CoV-2 anti-N IgG chemiluminescence microparticle assay. We infer that 16.9% (95% CI [9.48%, 28.5%]) of all presumed P.1 infections that were observed in 2021 were reinfections. If we also include cases of probable or possible reinfections (defined by considering the time period when the antibody levels are expected to grow after recovery and the range of half-lives for antibody waning after seroconversion), these percentages increase respectively to 25.8% (95% CI [16.7%, 37.4%]), and 31.0% (95% CI [21.4%, 42.5%]). Our data suggest that reinfection due to P.1 is common and more frequent than what has been detected by traditional epidemiologic, molecular and genomic surveillance of clinical cases.
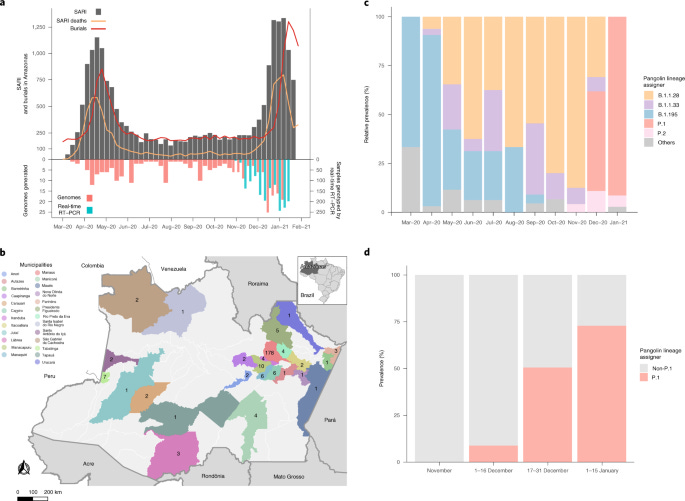
COVID-19 in Amazonas, Brazil, was driven by the persistence of endemic lineages and P.1 emergence
Through a genomic epidemiology study based on 250 severe acute respiratory syndrome coronavirus 2 (SARS-CoV-2) genomes from different Amazonas municipalities sampled between March 2020 and January 2021, we reveal that the first exponential growth phase was driven mostly by the dissemination of lineage B.1.195, which was gradually replaced by lineage B.1.1.28 between May and June 2020. The second wave coincides with the emergence of the variant of concern (VOC) P.1, which evolved from a local B.1.1.28 clade in late November 2020 and replaced the parental lineage in <2 months. Our findings support the conclusion that successive lineage replacements in Amazonas were driven by a complex combination of variable levels of social distancing measures and the emergence of a more transmissible VOC P.1 virus.