Risk of hospital admission doubled with Delta variant
SARS-CoV-2 Delta VOC in Scotland: demographics, risk of hospital admission, and vaccine effectiveness
In summary, we show that the Delta VOC in Scotland was found mainly in younger, more affluent groups. Risk of COVID-19 hospital admission was approximately doubled in those with the Delta VOC when compared to the Alpha VOC, with risk of admission particularly increased in those with five or more relevant comorbidities. Both the Oxford–AstraZeneca and Pfizer–BioNTech COVID-19 vaccines were effective in reducing the risk of SARS-CoV-2 infection and COVID-19 hospitalisation in people with the Delta VOC, but these effects on infection appeared to be diminished when compared to those with the Alpha VOC. The Oxford–AstraZeneca vaccine appeared less effective than the Pfizer–BioNTech vaccine in preventing SARS-CoV-2 infection in those with the Delta VOC. Given the observational nature of these data, estimates of vaccine effectiveness need to be interpreted with caution.
No COVID-19 cases found after well-controlled indoor concert
[Media report.] No attendees at an indoor concert that employed rapid COVID-19 lateral-flow screening, N95 respirators, and a well-ventilated venue tested positive for COVID-19 in the next 8 days, showing no increased virus transmission risk associated with the event, according to preliminary findings from a randomized, controlled trial published yesterday in The Lancet Infectious Diseases.
Evidence for lack of transmission by close contact and surface touch in a restaurant outbreak of COVID-19
We examined video data related to a restaurant associated COVID-19 outbreak in Guangzhou. We observed more than 40,000 surface touches and 13,000 episodes of close contacts in the restaurant during the entire lunch duration. There is no significant correlation between the infection risk via both fomite and close contact routes among those who were not family members of the index case. We can thus rule out virus transmission via fomite contact and interpersonal close contact routes in the Guangzhou restaurant outbreak. The absence of a fomite route agrees with the COVID-19 literature. These results provide indirect evidence for the long-range airborne route dominating SARS-CoV-2 transmission in the restaurant. We note that the restaurant was poorly ventilated, allowing for increasing airborne SARS-CoV-2 concentration.
Importance of wearing a mask continuously and appropriately regardless of the COVID 19 symptoms. Lessons from different mask-wearing styles among two healthcare personnel
The anecdotal report describes two examples of COVID-19-positive healthcare professionals (HCPs) who had worked as nurses during pre-symptomatic period and subsequently presented a mild clinical course of COVID-19. The nurses’ responsibilities were almost the same and worked in the general ward with no aerosol generating medical procedures. Two HCPs were expected to have similar infectiousness, but the number of secondary transmission by each HCP were different. Eleven close contacts from HCP1 were notified, and all of them tested negative for SARS-CoV-2. However, 13 of 35 close contacts of HCP2 tested positive for SARS-CoV-2. While working, mask-wearing style differed between the two HCPs. HCP1 wore a KF94 mask appropriately and kept wearing it while working. HCP2 wore a surgical mask while working, but often pulled it down to her chin or removed it. It was strongly suspected that the difference of mask wearing contributed to the SARS-CoV-2 transmission.
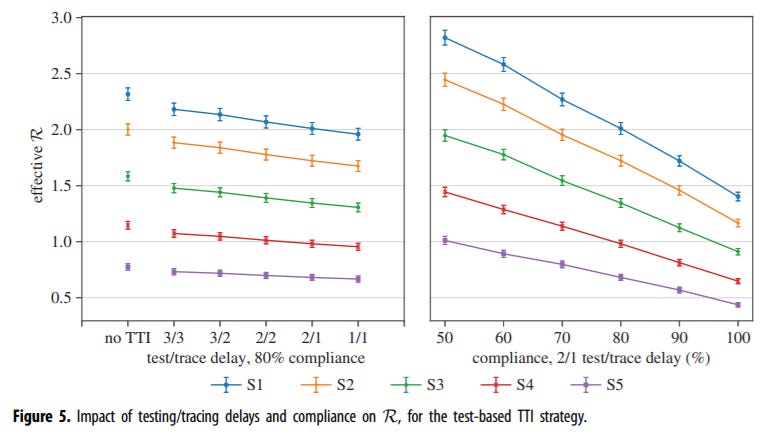
Effectiveness and resource requirements of test, trace and isolate strategies for COVID in the UK
We use an individual-level transmission and contact simulation model to explore the effectiveness and resource requirements of various test-trace-isolate (TTI) strategies for reducing the spread of SARS-CoV-2 in the UK, in the context of different scenarios with varying levels of stringency of non-pharmaceutical interventions. Based on modelling results, we show that self-isolation of symptomatic individuals and quarantine of their household contacts has a substantial impact on the number of new infections generated by each primary case. We further show that adding contact tracing of non-household contacts of confirmed cases to this broader package of interventions reduces the number of new infections otherwise generated by 5–15%.